
Photo/Jeff Frankel
By Amy Eisenhauer
EMS providers are injured or killed every year in ambulance accidents. It’s not a secret in EMS that sleep and provider wellness are secondary to the “mission.” We work long hours and spend a lot of time sitting in ambulances. We do this for love of the job and to make ends meet. Often agencies are understaffed and providers’ dedication to their fellow providers and patients make them stay long after shift to cover the shortfall. Our lives don’t start and stop when we punch in or out for our shift, we all have responsibilities outside of work, and those require our time and attention as well.
Its no surprise EMS providers are chronically fatigued, in fact, 35 to 40 percent of Americans are as well. The National Highway Traffic Safety Administration (NHTSA) cites approximately 91,000 traffic accidents were related to drowsy driving, with 50,000 injured and 795 dead from these accidents. A study in Austin, Texas, found that five percent of medics reported falling asleep while driving the ambulance and 50 percent having accidents or near-misses secondary to fatigue. Providers also have trouble staying awake while driving home from shift, inspiring Austin-Travis County (TX) EMS to build a “safe sleep room” for providers to nap undisturbed after his or her shift before driving home from work.
Fatigue doesn’t only affect providers operating the ambulance. Fatigue’s effects are insidious and touch all parts of our responsibilities as EMS providers. Sleep deprivation impairs attention, working memory, long-term memory, and decision-making ability. These effects can lead to medical errors, difficulties with ethical decision making, and being less vigilant in ever changing environments. EMS providers also have a 60% greater risk of injury when working shifts 16 hours or longer that shifts 12 hours or less.
Chronic fatigue also leaves providers predisposed to a variety of medical conditions including diabetes, obesity, cardiac disease, stroke, and increased morbidity and mortality. Chronic fatigue is strongly associated with depression, anxiety and post-traumatic stress disorder.
To help EMS agencies and providers combat fatigue and sleep deprivation in EMS, the National Association of EMS Officials (NAEMSO) has partnered with a research team from University of Pittsburgh School of Medicine to build The Fatigue in EMS Project. As part of this project, they have released five evidence-based guidelines for agencies and providers to use.
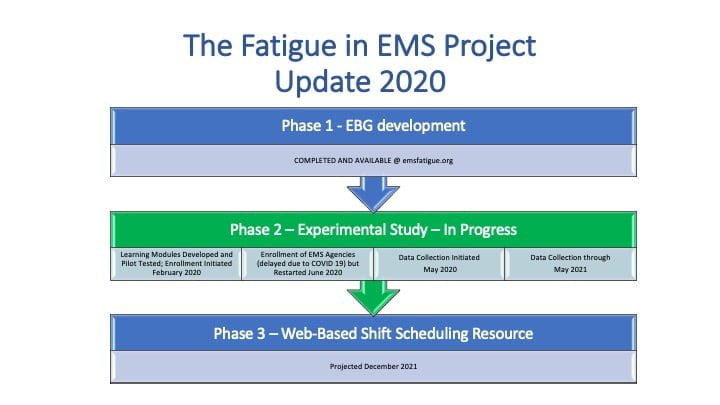
Image courtesy NAEMSO
- Measure and monitor fatigue in EMS personnel with a reliable fatigue and sleepiness survey tool.
- EMS personnel should work in shift shorter than 24 hours in duration.
- EMS workers should have access to caffeine as a fatigue counter measure.
- EMS personnel should have the opportunity to nap when on duty to mitigate fatigue.
- EMS personnel should receive education and training to mitigate fatigue and fatigue related risks.
While fatigue and chronic sleep deprivation in EMS providers is certainly a critical consideration in relation to safe ambulance operations, it is also critical to all parts of our mission. It is also critical that we care for our own physical and mental wellness in both the short and long-term for ourselves and our loved ones. The culture of EMS, and acceptance of fatigue as “part of the job,” only changes when we change it.
References
- Alhola, P., & Polo-Kantola, P. (2007). Sleep deprivation: Impact on cognitive performance. Neuropsychiatric disease and treatment, 3(5), 553–567.
- CDC Newsroom. 1 in 3 Adults Don’t Get Enough Sleep. Centers for Disease Control and Prevention. https://www.cdc.gov/media/releases/2016/p0215-enough-sleep.html.
- NAEMSO. Fatigue in EMS. National Association of EMS Officials. https://nasemso.org/projects/fatigue-in-ems/.
- NHTSA. Drowsy Driving. United States Department of Transportation. https://www.nhtsa.gov/risky-driving/drowsy-driving.
- Maxwell, R. (2016). Sweeping Plan Unveiled to Curb EMS Fatigue in Austin. Kxan News. https://www.kxan.com/news/sweeping-plan-unveiled-to-curb-ems-fatigue-in-austin/.
- Patterson, P.D., Weaver, M.D., Frank, R.C., Warner, C.W., Martin-Gill, C., Guyette, F.X., Hostler, D. (2012). Association between poor sleep, fatigue, and safety outcomes in emergency medical services providers. Prehospital Emergency Care, 16(1), 86-97.




