By Brent Smeins, Loren Ridge and Nicholas Nedza
There is the age old adage in emergency medical services (EMS) that if you, the provider, are uncomfortable in the back of the ambulance, the heat is correct for the patient. It is well understood that a patient’s temperature needs are much different from that of the EMS providers who are caring for them in their time of need. It is also proven trauma patients have higher morbidity and mortality if they experience hypothermia. The only option to keep the patient warm was to set the patient compartment heat to maximum. So EMS providers have been sweating through their uniforms in an effort to do what is best for the patient. At Waverly Health Center’s (IA) Ambulance Department, the question was asked, “What if we could heat patients differently?”
Smart Ideas
One of the best improvements that has been made at Waverly Health Center is the advent of huddle boards and daily huddles for the teams. Nowhere has this process been so embraced as in the ambulance department. For months, while awaiting shipping delays due to COVID-19, the EMS professionals gathered at every shift change in the hallway outside quarters in front of an imaginary board to talk about the shifts. Once the board arrived, this process improved significantly, including a section of the board for “smart ideas!” Every day it is asked by the manager if anyone has any “smart ideas” which can be added to the board. When suggested, they are put on the board with the provider responsible for seeing that idea come to fruition. Certainly, there are some ideas that are not able to be completed (we are still working on flying ambulances to avoid the bumps in the road), but they are all recorded. When the board is full, or the ideas get completed, they go onto a sheet in a binder for all to review.
It was during a daily huddle when a Smart Idea! was introduced to establish a better way to provide heat to a patient. Critical Care Paramedic Brent Smeins introduced an idea which could answer the question of temperature control for patients. He mentioned the idea of a Bair Hugger device in the ambulance, but knowing the size, space, and cost associated with one of these devices, suggested a different approach. The concept was introduced to remove one of the vents from the heating/cooling channel running above the patient and install a piece of hose which would then go directly into a Bair Hugger blanket.
Making the Connection
Being a hospital-based ambulance service has certain advantages, including the hospital having the Bair Hugger devices in the emergency department (ED) and therefore a supply of these blankets. They also had the hoses and connections to attach the blanket to the hose available for Brent and the Ambulance Department Educator, Lee Ridge, to look at and devise connections with PVC supplies from a local hardware store. Brent found the equipment necessary and worked with Lee to modify the connection to better direct the airflow from the removed ceiling vent into the hose and therefore into the blanket.
From this initial idea, some “dust debris” hose was obtained online and fitted to the PVC connectors. This allows the hose to screw into the threaded couple which replaced the ceiling vent. The threaded end of the hose also fits the blanket opening well and allows for flow into the blanket. With some zip ties and pop rivets, the hose connections were secured to the PVC coupler and could be quickly and easily screwed into and out of the ceiling vent.
The vent, which was replaced, is the rear most in the vehicle (by the patient’s feet on the cot) which allows for unobstructed treatment of the patient while in use. When not in use a plug is simply screwed into the open vent while the tubing and blanket are secured in an interior cabinet. When in use the hazard, should there be an unfortunate crash, is no greater than that of an IV bag hanging from the ceiling. The threaded portion in the removed vent is secured in place using epoxy and the tubing is screwed into that coupling. The blanket will then be covered by a traditional blanket which will then be under the cot straps ensuring patient and provider safety.
Testing It Out
When all the pieces and parts arrived, Brent and Lee assembled the devices and testing occurred in the ambulance. Brent’s daughter, Kerigan, an EMT with the department, served as the test patient. With the heat on in the patient compartment of the ambulance, airflow from the adapted hose inflated the blanket, much to the joy of Brent and Lee. The airflow increased the heat directly to Kerigan. Due to the ceiling vents having two channels, separated in the middle, one-half of the vents are unaffected and can stay open to heat the patient compartment of the ambulance while the vents on the side with the device can be closed to increase the flow of air to the patient.
By opting for the use of the ceiling vents the patients can now be both warmed and cooled without altering the temperature in the patient compartment, while also maintaining a comfortable temperature for the EMS staff. Closing all of the other vents in the patient compartment allows for the patient to be the only person who experiences a change in temperature. In Iowa, much like many places around the country, the ability to warm and cool a patient independent of the patient compartment is rather important and is now possible with this simple solution.
Below you will see photos of what was used and how the pieces are put together to create this heating and cooling system so you too can use this Smart Idea! Once the system was constructed and put into place it was tested in the following manner. The ambulance was pulled out of the ambulance garage so it could be run. The temperature of the bench seat, linen sheet on the cot and the counter of the ambulance was found. The heat was then turned on to max heat for five minutes and the temperatures were taken on these same surfaces again. In addition, the temperature of the heating and cooling blanket was read as well. After these readings the temperature was turned to max cool. Temperature readings were recorded on the same surfaces at five minutes and at ten minutes. The results are in the table below. What it showed was that the ambient temperature in the patient compartment stayed relatively stable while the patient could be independently heated or cooled.
Smart ideas like this can come from everyone and when people feel able to bring forward ideas, no matter how small, they can have a big impact on patient care. For more information on how this idea turned into reality please feel free to reach out.
| Initial Temp | 5 min Heat | 5 min Cool | 10 min Cool | |
| Bench seat | 66.2 | 71.6 | 71.1 | 69.6 |
| Cot linen | 69.1 | 86.4 | 77.4 | 67.1 |
| Temperature Blanket | N/A | 90.1 | 72.0 | 64.2 |
| Counter | 68.4 | 71.6 | 71.2 | 70.0 |
Photographs

Ceiling vent with flow directional louvers removed. (Photos/Nick Nedza)

Plug insert when hosing not in use.

Vent with hose in place.

Blanket with system functioning.
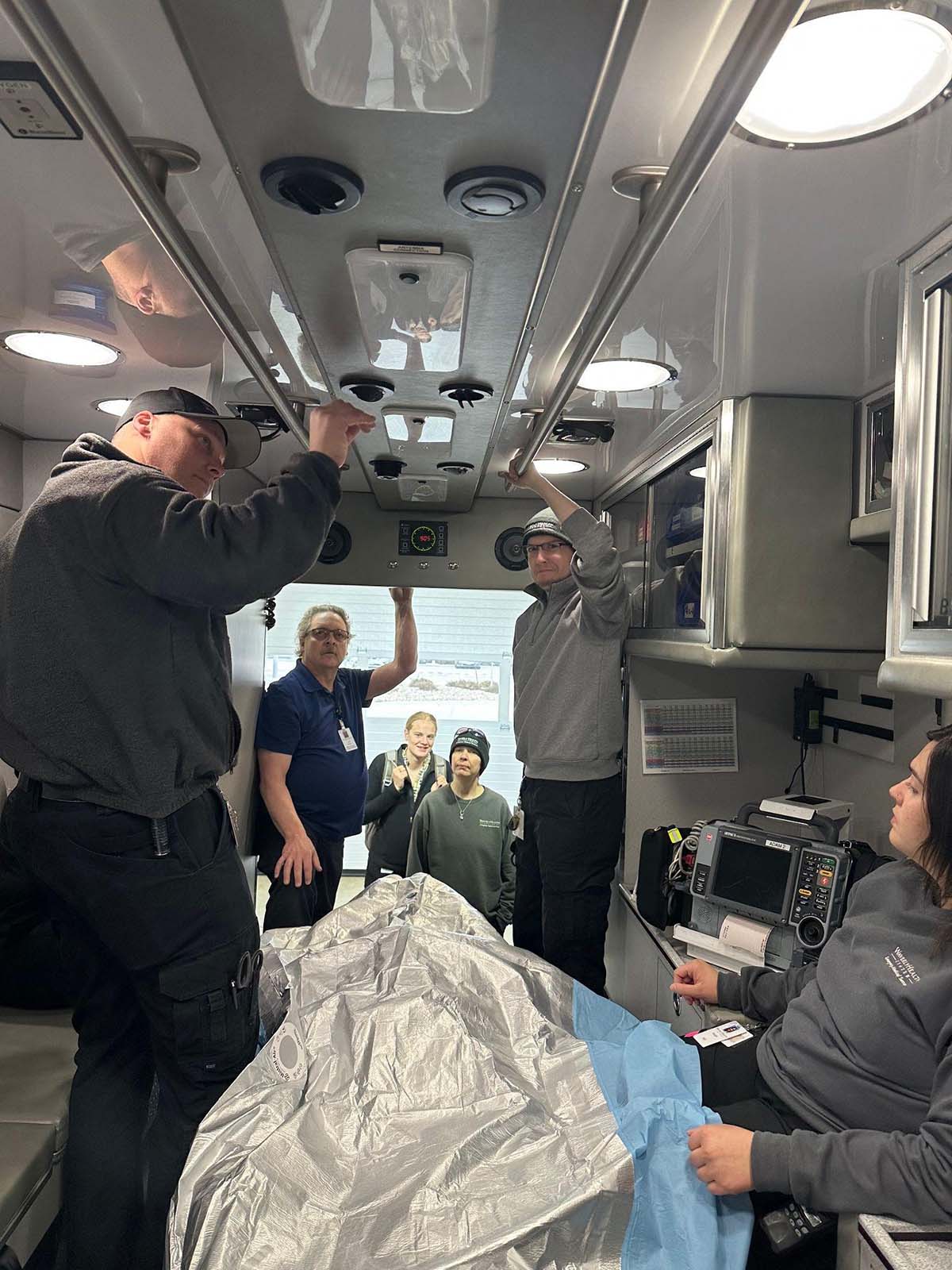
Demonstration by the design team to other EMS staff. On the left of the picture is Brent Smeins and moving from left to right is Lee Ridge. These are the two people responsible for the design and implementation of the system.
Brent Smeins, EMT-PM, CCP, is a critical care paramedic and has been involved in EMS and the fire service for 32 years, working for various services in Northeast Iowa. Currently, he works for Waverly Health Center in Waverly Iowa in the EMS department as a staff paramedic.
Loren (Lee) Ridge, EMT-PM, CCP, NCEE, FP-C, is currently the unit-based educator for Waverly Health Center’s Ambulance Department. Lee has been a Paramedic for 40 years and has served as a paramedic on both volunteer and career services, a flight paramedic, full-time educator, conference presenter, contributing author and a simulation specialist.
Nicholas Nedza, MBA, FP-C, CCP, NRP, EMT-PM, CHEC-II, is the ambulance department manager at Waverly Health Center, in Northeast Iowa, and host of the EMS: Always There to Serve Podcast produced by Waverly Health Center. Nick is a former flight paramedic at UIHC’s AirCare and is currently pursuing a Doctorate of Health Administration from A.T. Still University.




